Eczema
TOP TIPS FOR MANAGING ECZEMA
- Moisturise your skin twice a day every day even when there is no eczema and your skin looks or feels great.
- Use your medicated eczema creams or ointments as prescribed by your doctor or nurse practitioner – they will help.
- Try to wear cotton clothing where possible and avoid fabrics that irritate your skin.
- Turn long hot showers into short warm ones and pat (don’t rub) your skin dry. Be sure to apply medicated creams/ointments and moisturiser after you shower.
"It’s important to manage your eczema every day"
This project is proudly supported by an independent grant from Sanofi.
With eczema (also known as atopic dermatitis), the skin doesn’t hold moisture very well and dries out easily. It is important to keep the skin well hydrated with twice daily moisturising. This also stops substances in our environment, like pollen and animal dander, getting through the skin causing flare ups.
Few people understand the impact that eczema can have on your life…
- A rough night’s sleep because of the itch – we hear you.
- Feeling self-conscious around your friends – we get it.
- Feeling annoyed when you have another eczema flare-up – we understand.
- Shiny skin because of the moisturiser your skin desperately needs – we know it’s not the look you want.
Some things to know about eczema:
- There is no cure for eczema, but most of the time it can be managed really well.
- Eczema can be triggered by your environment. Irritants such as such as cleaning detergents, shampoos and washing powder, but also changes in weather and stress levels can trigger eczema.
- Scratching often makes eczema worse and we understand the need to scratch is hard to resist.
- You can’t ‘catch’ eczema.
- People with eczema often also have other allergies such as allergic rhinitis (also known as hay fever), asthma or a food allergy.
It is really important to manage eczema by following advice from your doctor or nurse practitioner. This helps prevent flare-ups and infections.
EVERYDAY ECZEMA MANAGEMENT
- A warm (not hot) short bath or shower daily for less than 5 minutes with a soap-free wash or oil.
- Apply moisturiser at least twice a day to your whole body and face, including straight after having a bath or shower. Apply moisturiser more often if your skin feels dry.
- Moisturise every day even when there’s no eczema. Moisturising helps prevent your skin from drying out and helps prevent flare-ups.
- Boost your moisturising efforts during the winter months as the cold, dry air can worsen your eczema.
- Avoid known triggers and things that irritate your skin such as soap, perfumed products, overheating, over dressing and prickly or synthetic fabrics (such as nylon, spandex) where possible. Choose loose fitting cotton clothing that doesn’t rub on your skin as you move. Rinse off salt after swimming in salt water and minimise direct skin contact with grass, sand and carpet.
HOW DO MOISTURISERS HELP MANAGE FLARE-UPS?
Our skin provides a barrier that helps control temperature and hydration.
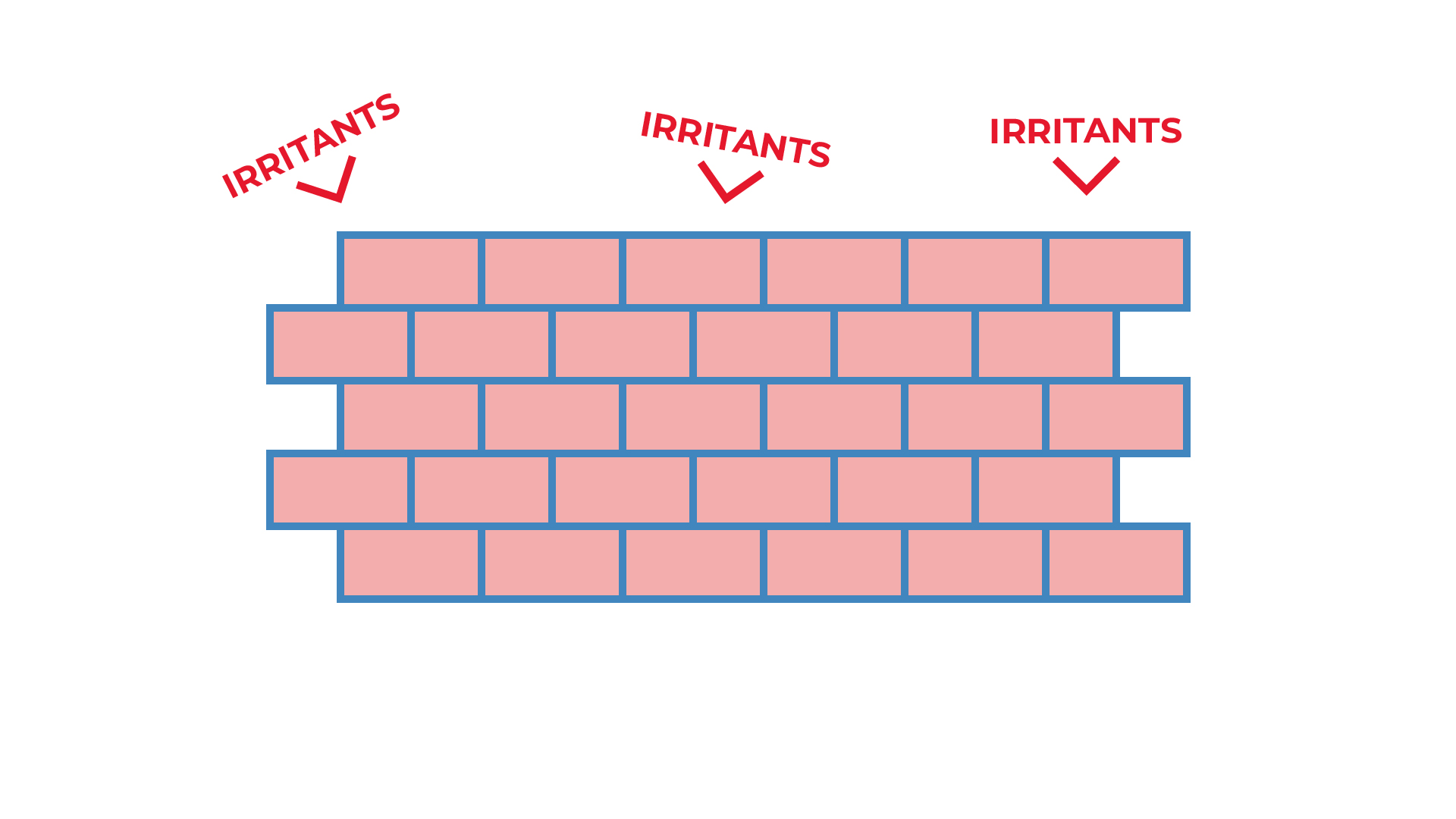
Our skin also helps to stop harmful substances entering the body. In people with eczema the skin barrier, does not work as well and the skin tends to be dry and itchy.
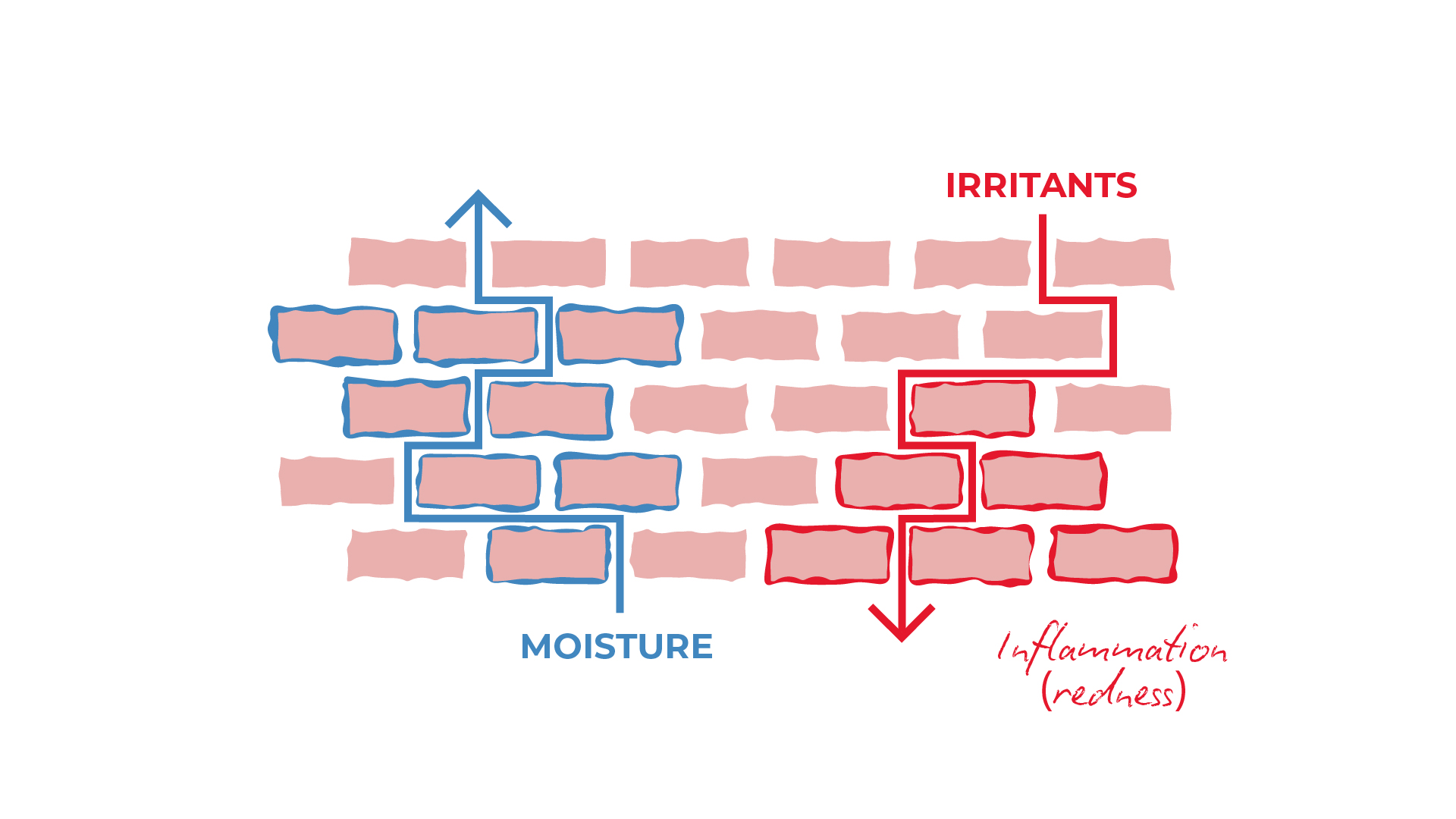
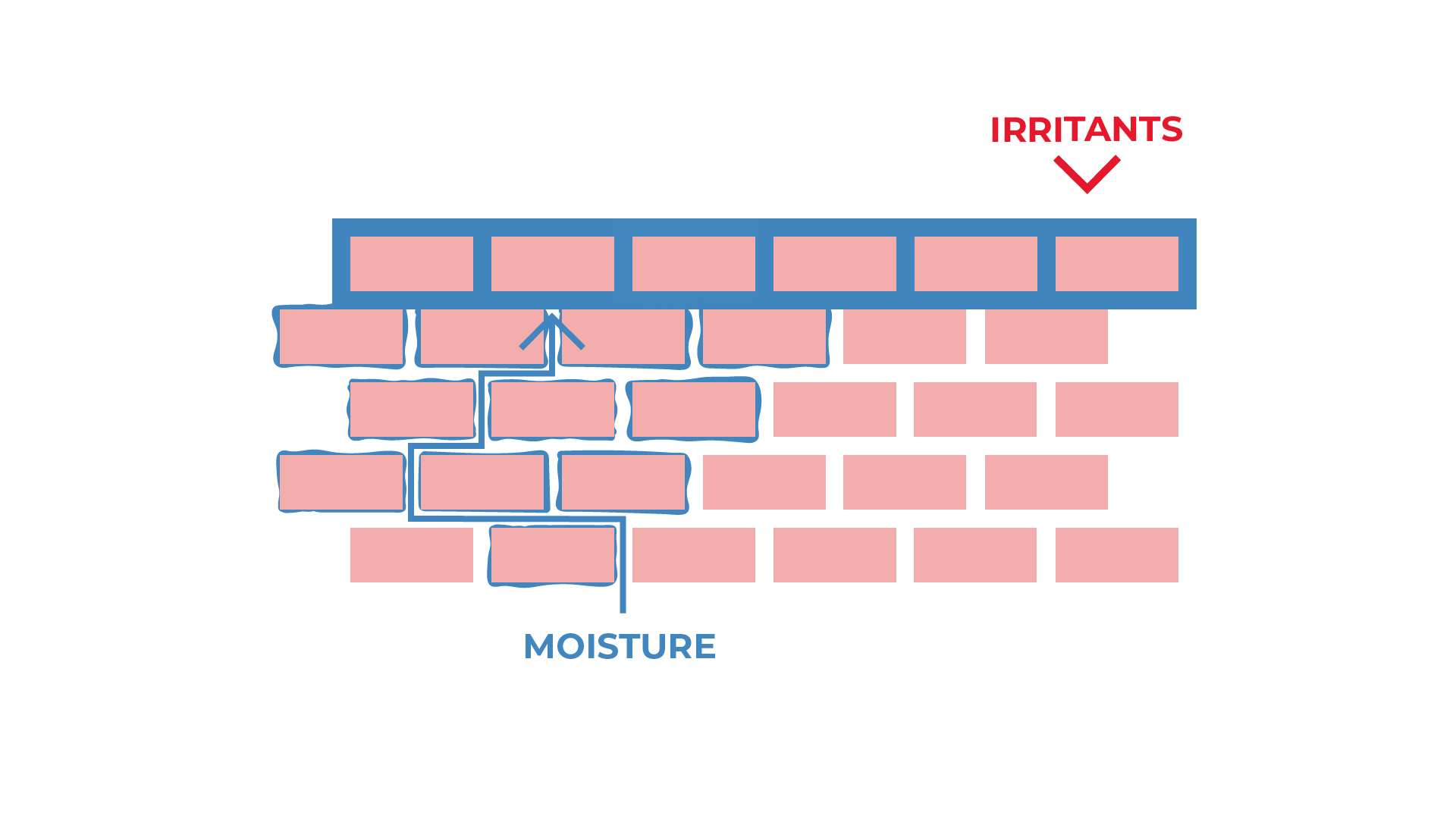
Frequent use of moisturiser is important to improve and maintain the condition of the skin.
Moisturisers fill the gaps between the skin cells, which reduces water loss from the skin and increases moisture in the skin. It can stop allergens such as pollens or food, getting through the skin.
MANAGING ECZEMA FLARE-UPS
An eczema flare-up is when an area of your skin gets worse than it normally is. It might become redder, itchier or feel more dry or rough.
When there is an eczema flare-up, your doctor or nurse practitioner may recommend the following:
Medicated creams or ointments
- Steroid and non-steroid creams or ointments to put on your skin where the eczema flare up is.
- These creams or ointments should be applied to all skin affected by eczema (red, itchy, dry rough areas including areas of broken skin) until the skin feels smooth and the eczema has completely gone.
- Apply moisturiser to your whole body and face after the steroid cream or ointment.
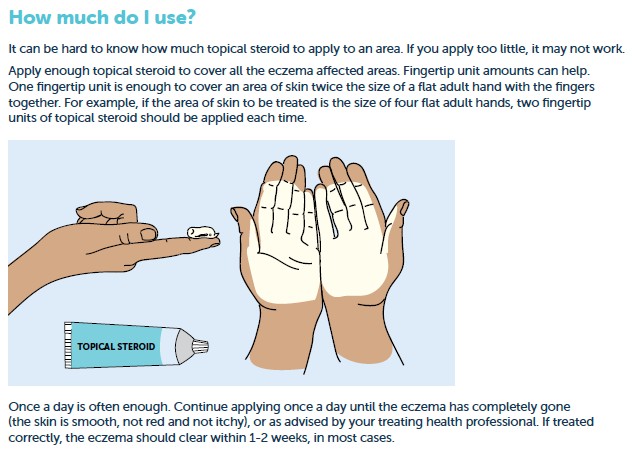
- Make sure you use the amount the doctor or nurse practitioner recommends so that you are treating the eczema well.
Wet dressings
- Wet dressings cool your skin, settle the itch and help eczema creams and ointments work better.
- They can be really helpful when your eczema is itchy and stopping you from sleeping.
- Your doctor or nurse practitioner will provide information about when and how often to use wet dressings.
- Learn more about how to use wet dressings.
Bleach baths
- Infections flare up eczema. Bleach baths are used to reduce the number of infections and improve the control of eczema.
- Bleach baths should be used as directed by your doctor or nurse practitioner for people who are prone to infected eczema.
- The final concentration of bleach when diluted in water is similar to chlorinated swimming pool water.
- Learn more about how to use bleach baths.
Other medications
- Other medications such as antibiotics and antihistamines may be advised by your doctor or nurse practitioner, although antihistamines aren’t usually recommended.
- Biologics are now available for severe eczema. They are restricted medications that are only used when other treatments have not been effective.
Acne and eczema
Teens and young adults generally have a tough time with their skin because of hormone changes. Some people have acne and having eczema too can be extra challenging. Taking good care of your skin can help with both acne and eczema.
Some tips include:
- Follow a skin care routine of cleansing the face using a gentle soap-free wash once to twice a day – don’t scrub or use harsh cleansers. Don’t forget to moisturise after cleansing and use an oil-free moisturiser on your face.
- Try not to scratch eczema and resist the temptation to pop pimples.
- Try not to wear makeup, but if you do wear it, try a small amount on your skin first , either on your forearm or an area where there is no eczema, and leave it for a few hours to make sure it doesn’t trigger your eczema.
- Protect your skin from the sun – check with your doctor or nurse about which types of sunscreens are suitable for people with eczema.
Depending how bad your acne and eczema are, you may want to see your GP and get a referral to a dermatologist.
Sport, exercise and eczema
Getting involved in sport and exercise can be a great way to get your mind off the itch and help manage stress. Choose activities which don’t cause more discomfort with your eczema.
Some tips include:
- Cover up with a hat and long sleeve clothing to protect your skin.
- Use sunscreen to protect uncovered skin from daily UV exposure when outdoors. Check with your doctor or nurse practitioner about which sunscreens to use. If your eczema is severe and you need to stay out of the sun, find activities that you can do indoors so that you don’t need to use sunscreen.
- Exercise indoors in air conditioning if sweating makes your eczema worse. Be aware that the air conditioning can also dry your skin.
- Swimming in chlorinated pools can dry out your skin but the chlorine can also help eczema as it’s like having a bleach bath. Apply moisturiser before and after swimming where possible.
- Shower after sport to remove sweat as well as after swimming and reapply your moisturiser.
Further information and support is available
There are organisations that you can contact if you need support with managing your eczema.
"It’s important to manage your eczema every day"

